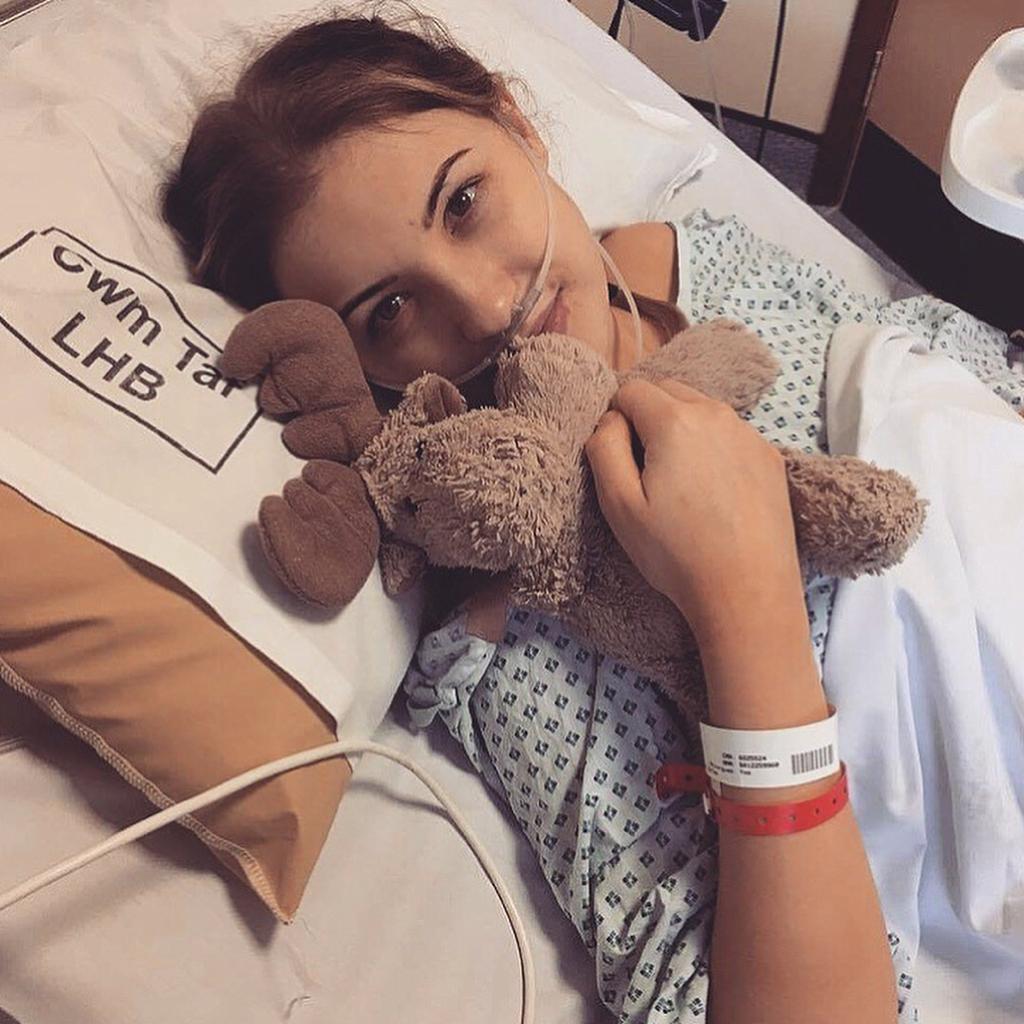
Amber’s Young Diagnosis Story: Age 13
Where do I start?
What is the biggest, most significant concern as a young teen?
Being late for the cinema? Not being able to get a lift to a friends house? Wanting a mobile phone?…
For me, I certainly didn’t anticipate it being a lifelong, chronic diagnosis or, the prospect of losing a major organ and wearing a stoma bag for a permanent accessory – what even is a stoma? (How clueless I was!)
I can’t actually pinpoint the beginning of my journey with Ulcerative Colitis – maybe because I was a little naïve, maybe because I was a little reluctant or, maybe, because my symptoms have been a part of me for as long as I can remember?
I believe, that it’s a mixture of all of the above.
The diagnosis…
Looking back, I’ve suffered with random symptoms of Ulcerative Colitis for as long as I can remember (mouth ulcers, skin irritation, tiredness, concentration problems, joint pain, low immunity, sore eyes) however, nothing that seemed overly concerning or abnormal enough to seek advice – I just got on with it and accepted it normal. In fact, I remember my earlier childhood as a happy and relatively healthy one. It wasn’t until my symptoms began becoming more noticeable at about age 11/12 (weight loss, extreme fatigue, numerous bathroom visits per day) that we, my parents and I, considered there may be an issue and it might be sensible to seek some advice?
No, ‘nothing wrong’. Why would you question the advice of a medical professional? In fact, numerous medical professionals.
Time after time I was told that these things were ‘normal’ for someone of my age to be experiencing, ‘it will pass’, ‘you need to be more accepting, most of it is in your head’, ‘you’re too young for there to be anything seriously wrong’.
I was rather embarrassed and felt ashamed of myself for what I felt like wasting peoples time and lacking ability to put up with symptoms that I was led to believe, normal. I felt like maybe I wasn’t as brave as my friends and others my age because they seemed to be carrying on so easily and as a result, I didn’t speak to anybody about it. So, I just got on with it. Things got progressively worse but by this point, I was rather used to my new ‘normal’ and very good at disguising what was going on.
Coming from rural Mid Wales, access to specialist facilities are far and few between. I had a fantastic GP surgery and good relationships with all of the staff there as a result of spending A LOT of time in their company however, because there wasn’t anything proven wrong with me by the generic bloods etc (you know how it is), there wasn’t much they could do for me apart from give me the time of day to listen to me list my worsening symptoms and admit me to hospital fast tracking A&E every couple of weeks…
Following this, I finally got a referral to a paediatric specialist, which at the time, felt like a huge relief and a light at the end of the tunnel when I was diagnosed (or, misdiagnosed should I say) with skin allergy problems – I had huge belief that taking a spoonful of Piriton each day was going to be my cure!
I began missing a lot of time off school and spent an increasing amount of time in hospital which was difficult on everybody with the nearest hospital to home being over an hour away and, because of my ‘odd’ symptoms, mixed with my age, I didn’t belong to any particular category and therefore, any particular hospital ward so was often mixed among a huge range of patients and, some rather eye opening and scary situations for a 12/13 year old. By this point I was passing a lot of blood daily, sometimes leading to me passing out. I was visiting the loo 20+ times a day, loosing weight, strength, hair and above all, hope. I was both mentally and physically drained being told I had different issues by each different professional that visited my bedside varying from eating disorders to arthritis.
Although I didn’t know what Ulcerative Colitis was, its eventual diagnosis, aged 13, following numerous procedures (that I must add, we had to demand) revealed one extremely destroyed and struggling colon, riddled with IBD. I was probably very naïve at the time, I still didn’t really understand what was going on or, take the time to make an effort to understand. I was so glad to have a diagnosis which I believed at the time, was going to be followed by a cure. Needless to say, I soon learned that a cure wasn’t an option. I began putting hope into different treatments as I slowly worked my way through the list with very little knowledge of what was going into my system or how it might affect me in different ways which often lead to me feeling rather disappointed and upset when side effects kicked in while my symptoms still weren’t easing…
From GCSE’s and A Levels to an emergency surgery…
Fast forward a few years which followed a very similar path filled with many admissions, ambulance rides, treatments and tears later, I was still in a very similar, worsening condition that again, I had become very used to and very good at disguising. I tried my very best to continue as normally as I could, having to drop from 15 GCSE’s to 9, completed mostly from my hospital bed, I was determined try and be like my peers. I decided to continue to sixth form in the same school in which the staff had always been extremely supportive despite not fully understanding what was going on either. With A levels and, my perseverance to be as normal as possible, undoubtedly came worsened health. Despite being about 16 at this point, I was still completely unaware of what the next steps may be for me, what the full extent of Ulcerative Colitis was and ultimately, the direction my health was heading in. In the summer of 2015, I continued to try and keep up with my studies, exams, social life, a part time job and had planned myself a fun and busy summer. By this point, I was taking approximately 26 tablets per day with my symptoms continuing to worsen. When on a family holiday abroad, things hit rock bottom – having not experienced a single period of remission since my diagnosis about 4 years prior, my symptoms were at their worst. I couldn’t leave the hotel room and by the third day of the holiday, I couldn’t even leave my bed for the maid to clean – I visited the resort doctor which proved difficult with a language barrier and there was no way I was prepared to be admitted to a Turkish hospital. So, I decided to take things into my own hands and take doses of all the back up medication I had with me (always travel prepared) – no success. I booked an early flight home which needless to say, was rather traumatic. I got an airport taxi straight to my local hospital (I had to ask the poor driver to stop at near enough every service station en route to use the loo and even had an accident in his car!). I couldn’t have been more relieved to see the doors of my hospital at this point.. After this, I didn’t step foot outside for over 8 weeks – probably the most significant weeks of my journey.
During this period of time, I lost so much blood that I passed out cold and required numerous blood transfusions. I was eventually allowed to begin trialling some biologic treatments however, by this point, it was too late. A stoma nurse came to visit me, she had her hands full and dumped everything on the end of my bed including leaflets plastered in photographs of the elderly and numerous stoma bag samples. I didn’t even know what a stoma was let alone what the surgery consisted of or that this was the next thing on the cards for me. I was totally reluctant and devastated, I didn’t want to know a thing. She left some bits and pieces in my hospital room however, I didn’t lay eyes on them again.
The next thing I can properly remember after this is waking up a day or two later to the same stoma nurse (who I’d been pretty rude to previously) this time visiting me to help with my first bag change, what? I had undergone emergency surgery to form a temporary stoma, 2015 aged 17.
The recovery
With recovery, my health began to improve. Despite having been through such major surgery and having a long road to recovery ahead, I couldn’t have been more grateful for my stoma at this point – I had slowly began eating again, walking, and managing to hold conversations. It was amazing and as cliché as it sounds, I was so so appreciative of all the little things I was now able to begin doing again.
Over the next few months, I began slowly reintroducing things and returning to ‘normal’. Because of my surgery and recovery time, unfortunately I had to withhold a year of sixth form. However, this meant I was able to give myself the recovery time needed and slowly adapt to my new way of living. Having this time also gave me opportunity to properly consider my future now that having my ostomy promised more stability in terms of my health. I began researching universities and planning what it was I wanted to move forward in doing in terms of my education and career prospects as well as all of the fun things I’d like to do having felt I’d missed out over the previous years. I even planned my 18th birthday party from my recovery bed and made it my mission to make it out in time!
However, again on this rollercoaster, I discovered that even surgery isn’t even a cure to IBD – my UC continued to flare and play up in my remaining colon and rectum which again, lead to a new journey of trial and error in terms of treatments following a similar pattern to the previous with nothing really working. By now, I had returned to sixth form for my final year and had began applying to universities persistent not to let UC get in the way again…
Soon after, I woke following another emergency surgery. This time, a completion proctectomy, the procedure whereby they remove any remaining problematic colon and rectum, sewing this area shut. 2017, aged 19, my stoma and I became permanent buddies which I mark as the real beginning of my new lease of life.
Things I wish I’d have known, would have benefited from or, had more support with at the time;
- A general better awareness for IBD amongst everyone, including health professionals and, the general public
- A better knowledge, understanding, awareness and approach for IBD particularly in hospitals and paediatric care – young people can have bowel disease too!
- More information and research with regards to IBD treatments for young people
- An improvement in the taboo/stigma that surrounds bowel disease
- More representation of influential people demonstrating that you can still do and achieve with IBD and/or an ostomy and less focus on IBD and ostomies being exclusively elderly and a matter of ‘end of life’
- Better inclusion of young people in their own care plans
I feel that I was very much kept in the dark when it came to my treatments and care. I feel as if I was very much kept protected from the harsh reality and truths of the extents of the disease and the treatments and that this isn’t always the best way. I would have benefitted from being told more, made more aware and generally being a part of my care plan rather than only finding things out at the last minute when at breaking point.
- An earlier introduction and discussion surrounding surgical routes with a perspective that surgery isn’t actually the end of the road or last resort and actually, can be a game changer with a positive outcome/future
- It may be an obvious one to some, but it is something I wasn’t ever told properly; there is no cure to IBD including surgery. Surgery has been a huge help and in fact, saved my life however, hasn’t eliminated all symptoms of IBD from my daily living – something I feel is very important to make people more aware of.
Amber
X
Visit Amber’s Instagram page here
Meet the blogger: Amber
Amber …..