International Nurses Day 2020: Interviewing Two Amazing Bowel Disease Nurses
Tuesday 12th May is International Nurses Day, which also marks the birth of Florence Nightingale in 1820. During the Crimean War, she was put in charge of the nursing for both British and allied soldiers in Turkey. Brittanica.com explains how Florence Nightingale also played a huge part in setting up training for nurses & midwives in workhouse infirmaries. International Nurses Day helps to remember her for her hard work & also focuses on the importance of a nurse’s role within healthcare.
With everything going on right now with the Covid-19 pandemic, it also highlights just how important nurses & it’s so inspiring to see so many of them selflessly putting themselves in harm’s way to help save the lives of others at such a scary time.
In this post, two inspiring Inflammatory Bowel Disease nurses selflessly gave me their time to ask them some questions (via e-mail) & kindly agreed to be featured. Read on to find more!
The importance of nurses within my Bowel Disease journey & stoma surgery
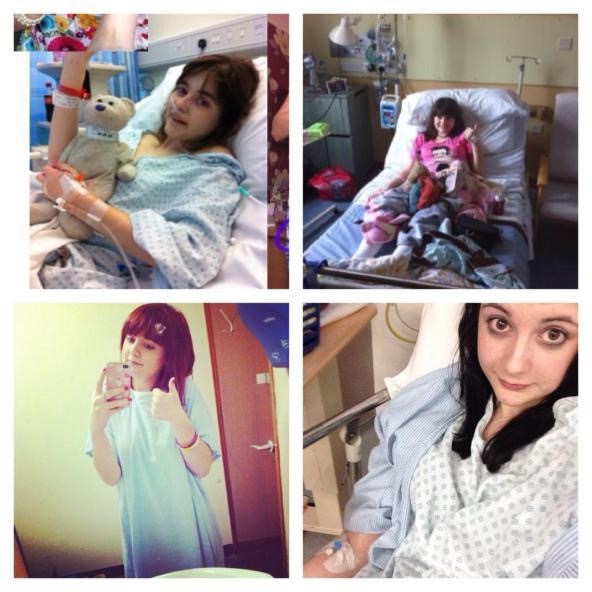 Even prior to my Crohn’s Disease diagnosis at age 7, nurses have helped make a petrifying journey less daunting & have done so many things for me. They have given me the courage to have painful tests, been a shoulder for me to cry on, hugged me when I was a child in hospital and couldn’t calm down, washed my hair when I’ve been unable to do it myself, given me smiles during my hospital visits and stays & they’ve even cleaned faecal vomit up from my body, my hospital bed and everything in its path!
Even prior to my Crohn’s Disease diagnosis at age 7, nurses have helped make a petrifying journey less daunting & have done so many things for me. They have given me the courage to have painful tests, been a shoulder for me to cry on, hugged me when I was a child in hospital and couldn’t calm down, washed my hair when I’ve been unable to do it myself, given me smiles during my hospital visits and stays & they’ve even cleaned faecal vomit up from my body, my hospital bed and everything in its path!
Alongside surgeons who have physically saved my life, nurses have made the difference between life and death for me, especially on a mental level. If it were not for the nurses being there in hospital in my darkest hours, I’d have struggled to see myself being here to write this.
My current stoma nurse is absolutely amazing & she always makes sure she has a space in her schedule to either see me or chat to me if I am struggling with any aspect of stoma life. She is an absolute star & is always on hand for a hug when I see her (apart from when you are social distancing, of course!)
As mentioned above, I was lucky enough to ask the below nurses some questions about their Inflammatory Bowel Disease worlds.
Emily – IBD Clinical Nurse Specialist (Instagram: @thegutsynurse)
Tell me a little bit about yourself?
Hello, my name is Emily! I am 29 years young and am from the Midlands. I am a gastro nurse by background, qualifying just over 6 years ago. I am proud to say I have since specialised in IBD, as a Clinical Nurse Specialist. Since becoming an IBD nurse I have ironically also been diagnosed with IBD and am now also a Crohn’s Warrior! Other than work I love running, yoga and cooking!
 What made you want to become an IBD Nurse?
What made you want to become an IBD Nurse?
From a young age, I always wanted to become a nurse. I spent lots of my teen years in hospital and I remember how amazingly inspiring the nurses were who looked after me.
After qualifying as a nurse, I have always worked in Gastro, but I knew my main passion was for IBD and desperately wanted a role in this field. I love the fact that IBD is complex and challenging and ongoing research gives it an ever-evolving nature. However mostly it was the patients that truly inspired me to do this role, the strength and determination they live with every day shone through. Looking after people with chronic illnesses is a lifelong journey, and both us and the patients go through that journey together. It takes empathy and understanding and having IBD myself now has helped me to build this more so.
Within your role, are you involved in a patient’s surgery journey? If so, at what stage do you become involved and until when?
I often see patients on the wards if their medical treatment is not working and it looks like they may be heading for surgery. Patients often deal with surgery better if they are mentally prepared and therefore, I believe this is a concept that should be discussed at the earliest stage possible with the patient. I know I would if it was me! I often provide psychological support and education if this is wanted. Sometimes just being a listening ear can really help patients come to terms with having surgery. I often see patients post-surgery to follow their journey and be that continued familiar face. Long-term management post-operatively often also involves a preventative treatment like a biologic to manage any future reoccurrence and again this means they get to see that familiar face.
Do you have any tips for those awaiting bowel surgery/hospital admission? 
For anyone awaiting either of the above I would suggest taking every day as it comes as looking at the bigger picture and questioning the future can occasionally provoke anxiety and uncertainty. Sometimes talking with other IBD warriors can help you see how other people have dealt with such challenging times and this can bring comfort knowing you are not alone on your journey. I would also advise reaching out to your IBD team, it is ok to not be ok and we can help you if we know you are struggling. Always take your home comforts into the hospital; iPads, furry blankets and your comfy pillow are all allowed and can make it feel more like home from home. I know this helped me when I was an inpatient myself!
Which part of your job do you like the most and why?
There are lots of parts of my job that I love but my most favourite has got to be seeing anyone improve. We know that IBD is a relapsing and remitting condition and there are lots of our patients who are now so thankful and well. It is truly lovely to see a patient who has been struggling, turn a corner and get them into remission. Often the journey can be winding and turbulent but when we get there, we have gotten over the hurdles together.
Which part of your job do you find the hardest and why?
The hardest part of the job for me is the emotional side. I try not to take my work home with me, but sometimes when you are on a journey with your patients, you truly do care! When things are tough for them, it can also be tough for us. I have a fabulous team and we are all there for each other- often we do have to have chocolate biscuit therapy!
 What is the one thing that stands out that your job has taught you?
What is the one thing that stands out that your job has taught you?
Being a nurse has taught me how resilient and strong humans can be! I see people day in and day out who are unwell taking it in their stride and continuing to achieve their goals. If they can do it, we all can!
Do you have any advice on those wanting to become a nurse?
Becoming a nurse was the best thing I ever did. I literally could not imagine myself doing anything else. If you have a passion to care and help others, then it is the right job for you. It is definitely not an easy job, but it’s worth all the hard work!
Any last comments you want to add?
Thank you for giving me the opportunity to speak out about the wonderful job of being an IBD nurse!
Thanks,
Emily
Kay – IBD Nurse Specialist (Instagram: @ibd_passport)
 Tell me a little bit about yourself?
Tell me a little bit about yourself?
My name is Kay. I am an Inflammatory Bowel Disease nurse at the Royal Free hospital in London. I have been a nurse since 2001 and I have been a nurse specialist since 2005.
What made you decide to want to become an IBD nurse?
I started my nursing career working on a gastroenterology ward for a year I then worked as an endoscopy nurse assisting with procedures such as colonoscopies and from there, I got my first role as an IBD nurse specialist. During my work in the other areas I developed a specific interest in inflammatory bowel disease. I also have an interest from a personal perspective having had Crohn’s from the age of 13. I think this did play some part in my desire to be an IBD nurse, but it wasn’t the main factor.
Within your role, are you involved in a patient’s surgery journey?
Yes, I am involved to some extent. I review patients in the outpatient’s clinic and therefore refer them to the colorectal surgeon I also sometimes attend surgical appointments with patients to be an advocate for them. I will also explain surgical procedures to any patients who may be undergoing surgery and I will refer them to the stoma care nurse specialist. Once the patient is admitted for surgery, I will review them whilst they are an inpatient just to make sure they are recovering well & to say “hello”, so they have a friendly face.
If you are involved in a patient’s surgery journey, do you play a role in helping them to recover mentally, as well as physically?
I ensure that I am always there for them to talk to I will go and say “hello” during their inpatients’ day and I will be a source of contact, in addition to the stoma care nurses during their recovery.
Do you have any tips for those awaiting bowel surgery/hospital admission?
My main advice is to not be scared to ask questions and to maybe try and talk to a friend or ask your IBD or surgical teams if they can put you in contact with somebody of a similar age to you who has also undergone surgery. This is a good way to find out what your recovery will be like and, in the case of having a stoma, practical tips on how to manage this.
Which part of your job do you like the most and why?
The part of the job that I enjoy most is the regular contact with patients. I really get to know them over the years and I often see them growing up getting married and having children. Because we see patients when they are well and when they are unwell, we get a good rapport and relationship with them and their families.
Which part of your job do you find the hardest and why?
The job can be very demanding, and I think a lot of people do not know the extent of what an Inflammatory Bowel Disease nurse does in their role. We must juggle a lot of different things in order to manage patients and keep the service running. Luckily, I have a good team around me to make this easier.
What is one thing that stands out that your job has taught you? (This could be about yourself, or people in general, for example)
The main thing that I have learnt is the importance of being patient and understanding and understanding my own limitations. In my role, we encounter people who are understandably anxious and concerned about their diagnosis and need reassurance. I have learnt ways of addressing people’s anxieties and also providing information in different ways to suit different needs.
Do you have any advice on those wanting to become a nurse?
Nursing is an amazing and rewarding career for anybody interested. I would advise discussing the role with any friends or family that they know who are in nursing to find out more about it. Some areas of work do offer things like work placements which may be useful. There is a shortage of nurses in the UK & there are many courses available.
– Kay
The importance of our NHS workers in the current Coronavirus Pandemic
On a personal level, I also wanted to also give a huge shoutout and “thank you” to our nurses and all NHS workers for their continued dedication, selflessness & hard work during this current pandemic. Every week, it is so lovely to see neighbours clapping with us for our carers & being able to hear clapping far & wide across town and seeing it nationwide on the news.
Thank you to Emily & Kay
Finally, I would like to say a huge “thank you” to Emily & Kay for giving me their precious time right now and agreeing to take part in my Q & A for this post. I thoroughly enjoyed reading about both your perspectives and nursing experiences & I’m sure others will have enjoyed it too.
– Amy









