So I have spent 20 years living with a chronic incurable illness, I am used to not always being in control of my body but the last couple of years have been difficult and during the first lockdown I finally got some answers as to what was going on after a barrage of tests to find out what was going on.
I don’t always openly post about my new condition but after spending 12 weeks with my first flare up and a few more in between I thought I would do some sharing.
What is Fibromyalgia?
Symptoms of fibromyalgia vary from person to person. The main symptom is pain all over your body.
There’s no cure for fibromyalgia, but treatments like painkillers, talking therapies and exercise programmes may help ease some of your symptoms.
It’s not clear what causes fibromyalgia. It can start after a stressful event like an injury, illness or the death of a loved one.
Symptoms
As well as widespread pain, people with fibromyalgia may also have:
- Increased sensitivity to pain
- Extreme tiredness (fatigue)
- Muscle stiffness
- Difficulty sleeping
- Problems with mental processes (known as “fibro-fog”), such as problems with memory and concentration
- Headaches
Irritable bowel syndrome (IBS), a digestive condition that causes stomach pain and bloating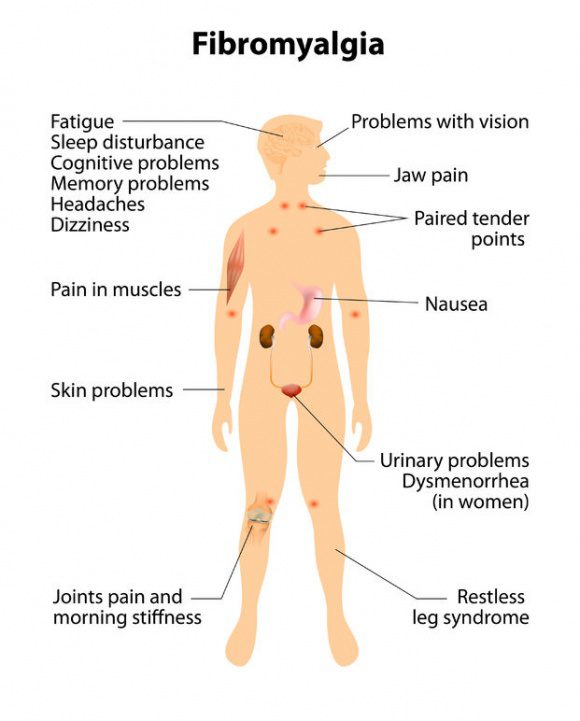 Photo credit: SpineUniverse
Photo credit: SpineUniverse
When did it start?
My fibromyalgia symptoms started about 2 and a half years ago, intermittent pins & needles, restless legs and twitching which was heavily impacting my sleep and I finally went for help when my legs gave out whilst I was having a shower.
It took a full year to get a diagnosis, I was referred to neurology, a rheumatologist and the foot people as I like to call them.
I had a fair few tests. MRI, CT SCAN, BONE DENSITY SCAN and some Nerve tests to see if I had trapped nerves that were causing the pins & needles. My MRI indicated that I have non inflammation based arthritis as well. I am still awaiting my appointment for surgical orthopedics as I need to have both my big toes broken and realigned due to bunions but that is another story to tell at a later date.
After diagnosis
After receiving the diagnosis I was referred to a physiotherapist. I’m still doing my exercises now as I have been advised that the best course of action is to keep on moving , even if it’s a little bit as muscle wastes and gets weaker which can exacerbate the symptoms. Laying about isn’t an option for me as I am incredibly stubborn and never quite do as I am told.
I have been referred for hydrotherapy and pain management clinic but due to covid this is still pending.
I attended an online self management course with the rheumatology nurses this tuesday just gone to explain the reason as to why I have fibro alongside tips and techniques to help manage the condition. I am under no illusion at some point in the future I will need a walking aid and possibly a wheelchair due to the ongoing arthritis. I am learning to live with it and it does occasionally impact my life and I get frustrated but it’s all a learning curve and I will get there in the end.
Basically my brain is broken, I may have made a quip about no shit Sherlock, like I didn’t already know, that’s just my way of dealing with things. The pain switch to turn off my pain no longer works, so there are times when I am in a lot of pain and other times when I am not. It also presents in other ways for me.
- I am clumsy and when I am flaring. I trip over myself, drop things, go off balance, fall over or walk into things
- I lose feeling in my legs and my right hand. I have been known to lose grip with a full cup of tea in my hands…
- Pins and needles. I get that sensation in my hands and my feet and my lower legs
- Insomnia. I struggle to sleep even though I need to sleep
- Pain. Some days I can’t bear to have people touching me as the smallest touch hurts me
- Muscle bunching and spasms. My muscles twitch and spasm of their own accord, this mainly affects my shoulders, lower back and my calves, sometimes my toes as well
- Brain fog. Sometimes it hurts to think
I am currently having my fibro treated and here’s what I do to help:
- Exercise and I am under a physiotherapist. I now keep to soft gentle exercise, so this is mainly walking and I also lift little weights to help my arms
- CBT. I have been referred back for a 8 week course to help change my mindset and also to help with my anxiety
- Self love. I am learning to take time out, even if its having a bath or an hour laying in bed, having time to relax has helped massively
- Learning and accepting that I can’t control things. If I need to sleep then I sleep, if I am having a bad day I work from home instead of going to the office
- Pacing myself, I have learned to pace myself. I can’t do everything, I now plan to have days off and weekends off where I just sleep, watch tv, walk the dog and chill out
Fibromyalgia is manageable, you can live with it. It’s like any other chronic illness, you have to learn to manage symptoms and take care of yourself so that you don’t have flare ups. I know that my c section and subsequent surgeries have led to my diagnosis, I have been on life support, fought 5 bouts of serious sepsis so this is the most likely reason as to why my body doesn’t perform like others. Like many with Fibro I am learning to live and juggle my various ailments and live the best quality of life that I can.
I have gotten a lot better with time, I now take my medication as I am supposed to, I listen to the professionals and I am also in tune with my body and listen and react to what my body is telling me. I will admit that I occasionally go off kilter, have a cry, have a rant, then I dust myself off, say it’s just one of those things and I carry on. My physio Gareth told me at the start of this that the more I move the easier things are and I have to admit that he is right, my good days and bad days are just those, even on a bad day I will still get up, walk the dog and then come back home and sleep, the exercise for me and the walking has really helped with my mental health and keeps me chipper.
If you ever want to talk or need some advice just send me a message, I am always here to listen and understand.
As always
Many thanks for reading
Louise Xx
Please note that this blog post is intended to give advice to ostomates. The information given is based on Louise’s personal experience and should not be taken as clinical advice. Please consult with your Stoma Care Nurse if you are in need of medical advice.

Meet the blogger: Louise
Meet Louise! She’s a blogger and ambassador for Pelican and has been for the last 3 years








