Simon’s Story: Ulcerative Colitis Diagnosis
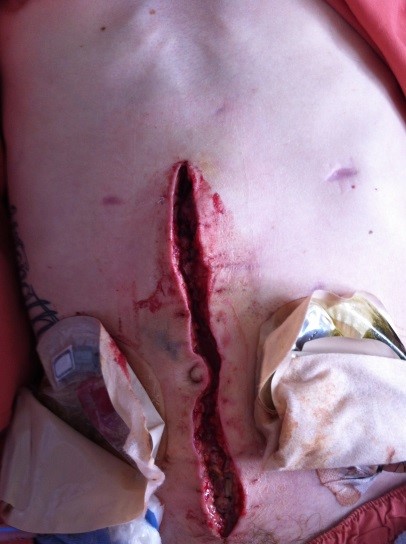
WARNING: this blog post contains some graphic images
So, where do I start? I guess the beginning seems like a good place, so here it goes…..
My name is Simon and I am 36 years old. I was first diagnosed with Ulcerative Colitis in May 2012. It was a relief to be diagnosed, which must seem weird to read but I went undiagnosed for years before diagnosis and the not knowing for me was much worse than finally having a name to my symptoms.
The months prior to my diagnosis were some of the toughest few months mentally and physically for me. In January 2012 I had keyhole surgery to correct a hiatus hernia; the surgery was called a Laparoscopic Nissan Fundoplication. After leaving the hospital following this surgery, my bowel symptoms seemed to multiply tenfold, I was regularly spending most of my days sat on a toilet, in pain and wondering what was happening. I would get the most excruciating pains in my stomach which I’ve only ever been able to describe as something similar to a washing machine spinning round tirelessly throwing clothes all over the place. The spinning and the pains were crazy; the only way I seemed to combat it was to lie down on my left hand side and curl my knees up under my chin. My fiancé (Natalie) at the time would often come home from work to find me lying on the floor in a random room screaming the house down in pain. It was at this point that we decided it was time to return to hospital to get some answers.
We attended A&E three times in as many months with the same symptoms every time; the first two occasions I was basically told there was nothing wrong with me and it was simply post-surgery complications that would ease, by the third time of being told there was nothing wrong with me, my fiancé and I decided to fight back and refused to leave without proper tests and answers. This is where my Ulcerative Colitis story really begins.
I spent a week in hospital on various drips and medicine to control the symptoms; during this time the staff requested a sigmoidoscopy, which is a camera examining the lower part of the large bowel, however this could not be completed due to the extent of the disease and the risk of perforation if continued. It was at this point that my Ulcerative Colitis was diagnosed and I was given a course of IV steroids for 5 days. My symptoms disappeared during those 5 days and I felt fine. A doctor spoke to me after the 5 days were up and explained they were stopping the IV steroids and if the symptoms remained dormant, then I would be sent home. They took the IV steroids down and left me watching daytime TV on my hospital bed. I don’t think it could have been much more than a couple of hours later however that the symptoms had returned, they came back so quickly after the IV steroids had been stopped that I hadn’t even had time to update my family.
As the hours went on, the symptoms got stronger and stronger to the point I needed IV painkillers to control the pain again. I managed to get some sleep between the pains and Nat was sat by my side waiting for more news. I was sent for a CT scan at midnight to check everything was okay, but despite the pain and the fact my symptoms returned shortly after stopping the IV steroids, at 2am the on call doctor woke me up to tell me I would be discharged in the morning. We were both relieved that the doctors felt they could control my symptoms with medication and follow up appointments would follow after discharge. I sent Nat home to get some sleep and told her to return in the morning to take me home. Off she went and back to sleep I fell, that was until…
At 6am the new on call doctor came to see me during his weekend rounds. He came to me first which surprised me as I was usually one of the last to be seen. I’ll never forget the first conversation we ever had and the words I heard being spoken to me but struggled to digest. He introduced himself as one of the hospitals colorectal consultant specialists (for the purpose of the story, I’ll refer to him as Mr H). He explained he had reviewed my notes that morning and understood that I had been informed of my diagnosis of ulcerative colitis and that I was told (again) only a few hours ago that I could go home today with medication to control my symptoms.
Unfortunately, Mr H wasn’t there to explain about my medications or wish me well with future treatments; he was there to explain to me that I wouldn’t be able to go home as in fact I needed to go for emergency surgery as soon as possible. He informed me that my large bowel was three times the size it should be and was completely infected. If he didn’t remove the large bowel within a few hours, I would die.
Mr H asked me to contact my fiancé so she could come in and also have a discussion with regards to what was happening whilst he was getting things sorted behind the scenes. I was in shock. I couldn’t believe what I was hearing and time felt like it stopped. Mr H left and I eventually picked up the phone to speak to Nat. She answered the phone sounding very bright expecting me to say come and get me. I repeated what Mr H had told me but probably not quite as well. I’m not entirely sure Nat believed me if I’m honest but she got straight in the car and drove to my parents’ house to explain the situation to them. She then drove straight to the hospital with my Mum to get the full details from Mr H. (I should probably explain at this point that Nat is a Nurse and she worked at the hospital where I was currently a patient at).
Once Nat and my Mum arrived, Mr H came and spoke to us all, explaining what he’d already said to me to Nat and my Mum, that I had Toxic Megacolon and even though I think we were all a little shocked. I knew right then that I was going to have the surgery to remove my bowel or die. Mr H explained that he would remove the large bowel, leaving my rectum and bring a part of my small bowel outside of my skin forming a temporary loop ileostomy. (I’d never heard of Ulcerative Colitis before a few days ago let alone stomas or ileostomies). The forms were signed and within the hour, I was on my way down the long corridors towards the theatre department, staring down the corridors I was admittedly a little nervous, I hadn’t really been in a situation like this before and it was all so sudden.
The surgery was called a sub-total colectomy and lasted approximately 8 hours. The reason for this was due to having to clean all my internal organs prior to starting as I’d leaked faeces internally. The bowel was then so damaged that they had to complete the procedure carefully, not to damage the small bowel. After the surgery I woke up, groggy and confused but Mr H was there to tell me and the family that the surgery was a success and it was now time to rest and recover. I was relieved. I could see Nat was relieved but we knew it wasn’t going to be an easy ride going forward.
We were of course due to be married in a month’s time, the church was booked, the reception venue booked, the guest list sent out. We were also expecting our first child; Nat was 3 months pregnant so I needed to recover and get home.
Unfortunately we didn’t quite expect the next bit and it again caught us off guard. A few days after the surgery, I became extremely unwell again. Nobody knew what was causing the symptoms but it was decided to take me back to surgery to have a look inside. I was taken back to theatre immediately and opened up again. At this point, it was found that my small bowel had perforated and I’d got septicaemia. They patched the small bowel up but due to the circumstances, I was placed into an induced coma. The surgeons spoke to Nat and my parents to explain what had happened and told them that the next 24 hours were critical and I only had a 50/50 chance of survival. 24 hours later, I woke up and there was another sigh of relief, however, again this was short lived as another few days later I was again extremely unwell.
A third trip to theatre for more surgery. Again my small bowel had perforated so they decided to bring some of that out and gave me a jejunostomy (second stoma).
I’d gone from no diagnosis to Ulcerative Colitis to one stoma and then two stomas, all within a couple of weeks and my head was struggling. I didn’t know what to think or what to do. I was a mess. Mr H would come and see me every day, multiple times to make sure I was okay. He used to tell me the same thing every time and at the time I used to think he was being stupid but looking back, it was great advice, he used to say to me: ‘You look after your head, keep that positive and I’ll look after your body’. I used to think he was mad, my body was in pieces and wasn’t showing any signs of being okay but slowly I started to realise that he was right: I needed to remain positive if I was going to get better.
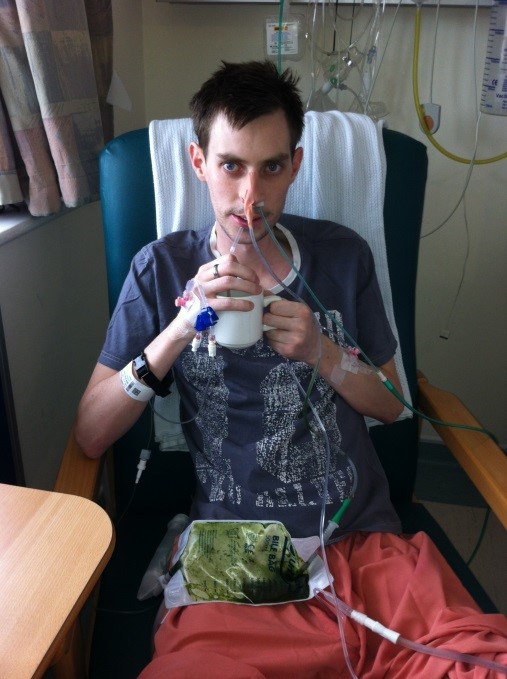
After a few days of resting following the third surgery, Mr H came to see us to discuss the plan going forward, the first question I asked was whether I’d be home in time for the wedding in 4 weeks. Mr H wouldn’t give me an answer but promised they’d do what they could to help me make the church in time. The days went by with constant medication 24/7 and although I felt okay, I knew I wasn’t getting better quick enough. I’d lost over 6 stone in the couple of weeks prior to surgery and I was 6 stone wet through at this point. I couldn’t eat due to the amount of surgery the body had been through so Mr H got the nutrition consultant to come and see me. Her name was Dr B and she immediately decided I needed help to eat; it was decided that I would have a central line put into my neck where the hospital would be able to administer total parental nutrition (TPN), this eventually became a Hickman line which I was fed through for almost 2 years in total.
It was becoming more and more apparent that the road to recovery was going to be a long one. I kept asking if I could go home so I could get married but eventually Mr H admitted that it wasn’t possible. I couldn’t even get out of bed two weeks before the scheduled wedding let alone get married. We were devastated but more determined than ever to continue with the wedding, so we did the next best thing and brought the wedding to us. We arranged to use the hospital chaplain and invited our guests to the hospital and we got married as planned. I wore a suit (a million sizes too big at this point), Nat wore her dress, and the bridesmaids wore their dresses. I was wheeled down to the chaplain in a chair and spent most of the time sat down, but I did manage to stand for the vows and we had a little dance. After the ceremony, we went back to the ward where we watched a film and spent the first night as Husband and Wife in my single bed.
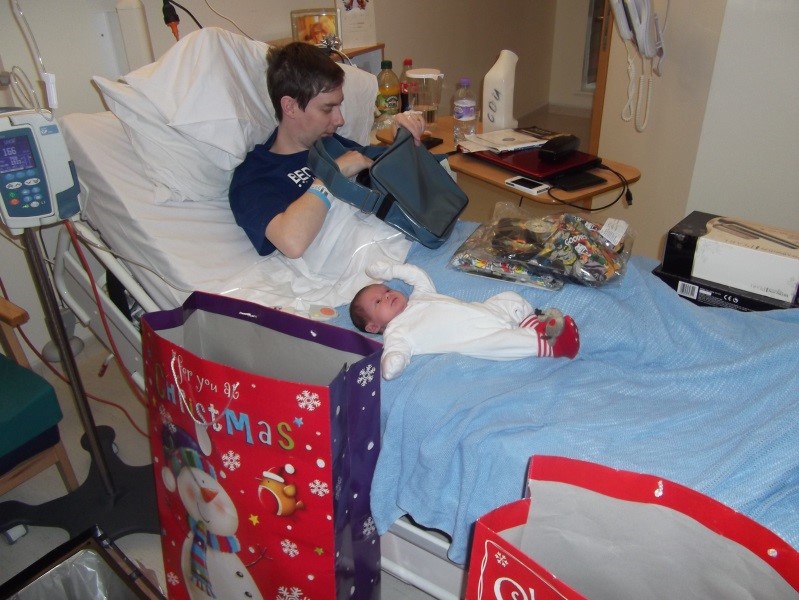
Now at this point, I have to be honest, I can’t remember all the details on a day to day basis but what I can tell you to shorten this story is that I ended up not only being in hospital for the wedding but also for the birth of our first child, a healthy boy called Charlie. Now I remember building up to this point, I had been in hospital for months and months, day and night, Nat was heavily pregnant with our first child and working full time at the hospital as a Nurse. I honestly don’t know how she did it. Coming into the hospital for 6-6.30am every morning to get me washed and ready for another day watching Jeremy Kyle on my hospital bed, then going down to her ward to work a full days shift, coming back to see me at lunch for a Jacket Potato and a kiss, then returning after her shift finished to sit with me for another hour or two before going home to sort the house out and crash in bed for a few days. I probably don’t tell Nat enough but I am eternally grateful for how strong she remained and for never giving up on me.
At the time of the birth the hospital let me go home for a couple of days but then I was straight back to the hospital to continue the recovery. I can’t remember the exact timing but I ended up being an inpatient at the hospital for approximately 10 months during my first stay, apart from a few days here and there. Let me tell you that 10 months in hospital feels like an absolute lifetime but the staff all became like family during that time. After those 10 months, I convinced the hospital to allow me home despite their reservations for me to continue TPN treatment at home under careful supervision of BUPA Nurses who would attend the house twice a day to assist with connecting and disconnecting the TPN to the Hickman line. Now this agreement was in place for a short time, where I had to prove I could stay healthy and gain weight. I thought that would be easy and I’d be laughing but within two weeks I was back in the hospital as an inpatient, after gaining no weight at all. I think I was in hospital for another few months this time around. If anyone has ever wondered, the hospital TV becomes rather expensive after a while!
During this spell, I had my second stoma reversed and I went back to having just the one stoma. I did name this stoma but if I’m totally honest, I changed my mind so many times that in the end I decided to have a nameless stoma.
During my time as a patient at this hospital, I had procedures and tests pretty much daily, from X-Rays to CT scans and MRI Scans. I had replacement Hickman lines from infections, drains hanging out of my stomach, NG tubes going into my stomach from my nose – you name it and I’ve probably had it.
The entire time though, one thing kept whizzing round in my head, yep, it was that line from Mr H:
“You look after your head and I’ll look after your body.”
I spent Charlies first Xmas in hospital; well I woke up on Xmas Day in hospital, Nat and Charlie came to visit and then they snuck me out, we went to my parents’ house for Xmas dinner and then we went home to our house. I slept like a baby in my own bed and the next day, we woke up and went back to the hospital refreshed and ready to keep the fight going.
Eventually I was well enough to be discharged, I left the hospital and we decided to renew our wedding vowels, we spoke to the local church and explained our story and they booked us in at short notice, we were also given the local football clubs stadium to host a wedding venue and invited all the original guests. We then went on a short honeymoon to Cornwall with Charlie.
As you can see, the weight is already starting to come back and I look much better than I did 12 months ago at the first wedding.
In 2014, despite Nat’s reservations, I decided to try J-Pouch surgery, which would have seen my stoma placed back inside my body and the ileostomy taken away. I was directed to have this surgery in Oxford, approximately 1.5 hours away from where I live. I had the surgery done but they left everything unconnected to let the healing begin. I was due to return three month later to complete the procedure and have it all connected. Unfortunately my body decided to mix things up again; it decided not to heal properly and instead decided to reject the J-pouch and send me back to the start line. This meant that in the end, I was referred to Birmingham hospital in 2016 to remove the J-pouch and return to the ileostomy, this time being a permanent one (still nameless).
2016 remains my last major surgery at present, however I estimate I’ve had approximately 10 major surgeries since diagnosis in May 2012. I have many scars to show for this, however I don’t see them as scars, I simply see them as reminders of the incredible journey I have been on (sorry we have been on as a family).
At the time of writing this story (June 2019), I have returned to work full time (in a restricted role as office based Police officer), I have gained all the weight lost back and more, I have trained for and completed the 2017 Great North Run half marathon (having never ran any distance further than 100 metres before). In May 2019, I completed the Yorkshire 3 peaks challenge in under the 12 hours (having no experience in hiking before) and I am already trying to decide my next big challenge.
I actively play football once a week and try to go to the gym two or three times a week to keep as healthy as I can.
I have a saying that I truly believe in, other than the one Mr H drilled into me, and that is that I control my Ulcerative Colitis, I don’t let it control me.
Yes I have bad days, I have hospital admissions from time to time, I spend my life looking for the nearest toilet or carefully planning my journey. I have to be careful what I eat and when I eat it, I have developed the most annoying OCD in the world, but I will never let these things bring me down. I will keep fighting the bad days and I will see more good days than bad.
Finally, the family became four. We had our second little boy (Sebastian) in March 2018 after years of trying, after years of being told it couldn’t happen and after once again proving that anything can happen providing you look after your head and remain positive.
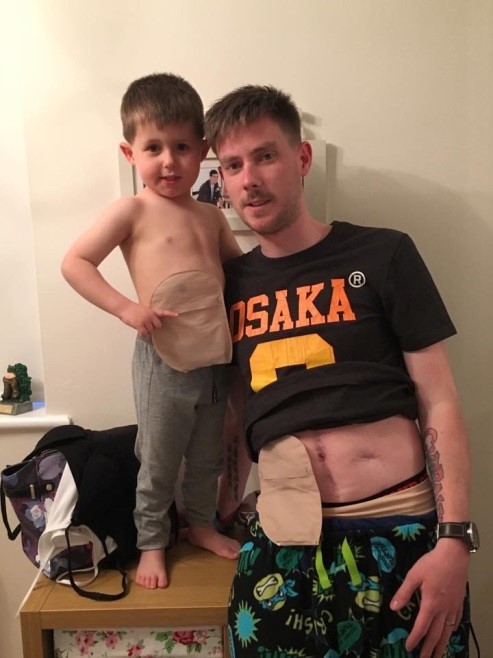
Charlie is now 6, he has grown up with me having a stoma and isn’t bothered by it at all. We call it my poorly and he knows to be careful of jumping on it but as you can see from the picture, he doesn’t let me having an ileostomy bag get in the way of our relationship. This picture was taken because Charlie said he wanted to be like daddy and have a bag, so we gave him wish (for a few minutes anyway). Charlie does also have a teddy bear that has a stoma and an ileostomy, the ileostomy bag is attached with Velcro so he can take it off and change it if it needs it.
So that’s it, that’s my story. I hope you’ve enjoyed reading my journey as much as I have reliving it.
Simon