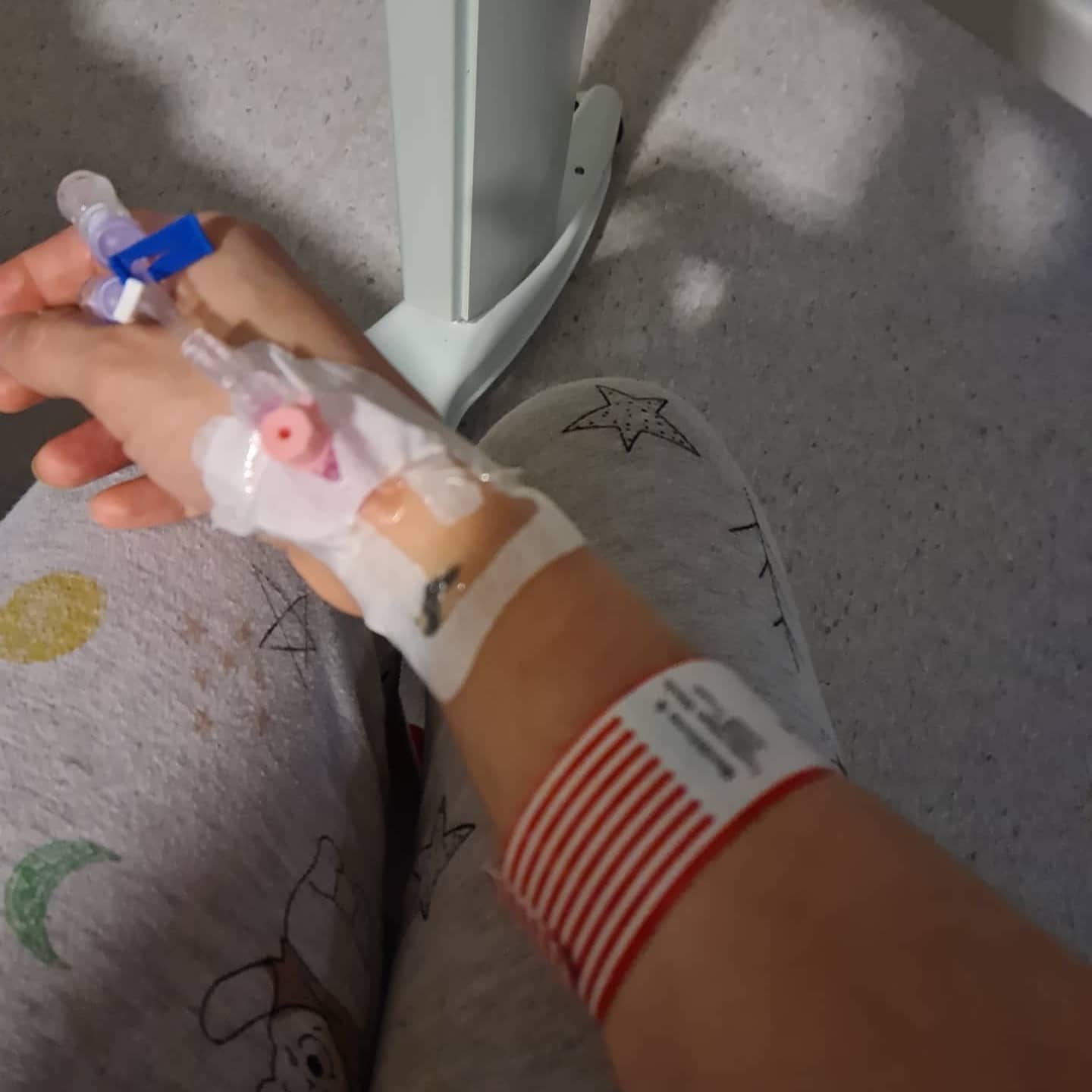
Stoma surgery doesn’t necessarily cure the owner of their ailments. For some it does… alas for me it has given me a few years of remission but hasn’t completely rid me of active Crohn’s disease. I have been having issues with ulcers on the end of my ileostomy since the first lockdown that keep coming and going and bringing back more friends to party. I have spent endless amounts of time emailing my IBD clinic along with photos and videos of said flare up on the end of my stoma.
Insta abdominal abscess & CT scan
I have had about 12 stoma nurse appointments in the last year, each referral back to the IBD team stating they are Crohn’s ulcers has fallen on death ears. The whole situation with Covid has not helped and I will be honest I avoided hospital until after my first Covid vaccine where I was admitted due to a rather large fetching intra abdominal abscess that had made me go septic again. Active inflammation was picked up on a CT scan in my duodenum. This has been frustrating for me. I know when my illness is active – fatigue, hair loss, active cramps, insomnia are just a few of the symptoms.
Thankfully my hospital appointment has led to a fair few active MDT meetings. After a video call with my surgeon last week and baring my stoma along with recent blood tests have confirmed active Crohn’s again (just what I need before our wedding). I now need a further test, an MRI to confirm how much active inflammation is currently sitting in my small intestine.
I am now due to go for my screening tests to start on Sterela before the end of August. If it’s not under control by January then I am booked back in with my surgeon to have my ileostomy refashioned and the active Crohn’s removed from that small portion of bowel.
You may be asking why not just have it cut out now?
My last CT scan revealed a collection behind my current stoma and my last ileo scope couldn’t get further than 8 cm up my stoma. There is either scar tissue blocking that part of the bowel or an internal fistula that is connected to different parts of the bowel. The area around my stoma site is still swollen and a little bumpy and I don’t have a hernia.
I am so happy with my stoma. It has for the most part kept my Crohn’s at bay. It is just slightly unfortunate that with the severity of my disease that it has now jumped ship to my healthy remaining bowel. My surgeon explained to me last week that the part of the small bowel that makes my ileostomy is from my original anastomosis site where it was last indicative of active disease. It was advised after my last surgery that I would need to be on lifelong immunosuppressant therapy to keep it at bay but my GI was reluctant to place me on anything whilst the disease was inactive.
If the Sterela doesn’t get the flare under control then I am booked back in with my favourite surgeon to have my stoma refashioned and the inflamed bowel removed. I am crossing my fingers and toes that the treatment works as I really do not want to have another surgery. My postoperative outcome after surgery is always torrid, not to aforementioned the sepsis after every surgery or the fact I have had post-op ileus every damn time.
What should you look out for?
Disclaimer: I am not a medical professional and all my blog posts are written from a first-hand perspective and are for advice and guidance. Should you experience any of the issues mentioned below please seek a medical consultation with the relevant team.
- Ulcers or patching on your actual stoma – they tend to be around the ileostomy including the underneath, patching and discolouration of the actual stoma ie, light pink, white or really deep red.
- Funky output, my stoma output has been crazy. I go from extreme watery output, to being constipated (madness but with active Crohn’s you can go from excessive bowel movements to none)
- Chills & or fever – a flare can cause you to run a fever or feel more flu-like
- Extreme fatigue, fatigue is also an indicator – I have really been struggling to get out of bed recently
- Mouth ulcers, ulcerated & or swollen gums can indicate a flare
- Bruising – I keep getting bruises and not knowing where they came from
- Insomnia. I either can or can’t sleep – being up all night emptying a flushing bag leads to sleepless nights, add in the relevant pain medication and I can’t sleep
- Unable to maintain weight – my weight has consistently dropped the last 8 months and has not stayed stable (weight loss is an indicator)
- Abdominal pain
- Cramps
- Bloating & wind
- Skin infections
- Hair loss
- Blood in stools
Here’s hoping the next couple of months and my first infusion gets this all under control. I am incredibly grateful that my consultant team have finally put together a game plan. The last 18 months have been incredibly hard for the NHS due to covid and I would rather deal with a flare than risk hospital at that time. I have been monitored closely and regular calls and updates have now finally got me the necessary treatment needed. Being on Immunosuppressants such as Sterela during the height of the pandemic was particularly scary and I would rather not have taken the risk.
As always
Many thanks for reading
Louise Xx

Meet the blogger: Louise
Meet Louise! She’s a blogger and ambassador for Pelican and has been for the last 3 years